In our Ask a Doc series, we sit down with physicians and other clinical experts, including those at Allegheny Health Network (AHN), for a chat on an important health topic. In this interview, Dr. Howard Edington provides insights on melanoma and skin cancer.
One in every five Americans will develop skin cancer in the course of a lifetime; one in every 50 will develop melanoma. And these numbers are increasing.
Howard Edington, MD, a surgical oncologist at Allegheny Health Network (AHN), is leading development of a new Melanoma and Skin Cancer Center at West Penn Hospital. Dr. Edington took time to talk with me about the basics everyone should know about skin cancer, some innovative ways of treating it, and how the center will be a hub for both cutting-edge research and convenient, coordinated care for patients.

Dr. Howard Edington, a surgical oncologist, is leading development of AHN’s new Melanoma and Skin Cancer Center at West Penn Hospital.
Emily Adamek: What are the different types of skin cancer?
Dr. Howard Edington: We can sort it into two baskets. Non-melanoma skin cancer is one basket, with 95% being basal cell carcinoma and squamous cell carcinoma. There are also what are considered rare cancers, including Merkel cell carcinoma. If you add up how many non-melanoma skin cancers there are per year in the U.S., it’s more than all other cancers combined.
Melanoma is the second basket. Melanoma cases have been increasing dramatically, for reasons that aren’t totally understood. It’s on track to become the second most prevalent cancer by 2040.
Emily Adamek: What causes these skin cancers?
Dr. Howard Edington: In non-melanoma cancers, most cases are associated with cumulative exposure to ultraviolet radiation from the sun. You typically see older people getting basal cell or squamous cell, and often they’re outside workers with a history of prolonged exposure.
The cause of melanoma is thought to be an interplay between genetic predisposition and environmental factors like sun exposure. But we are seeing a lot of young people getting it — it is now the most common cancer for people between the ages of 25 and 29. This could be due to episodic exposure, such as time spent in tanning beds or laying out on the beach — big blasts of exposure in short durations.
Emily Adamek: In addition to sun exposure and tanning beds, what other risk factors should we know?
Dr. Howard Edington: One risk factor is previously having had a biopsy showing atypia or atypical lesions. A personal history or family history of having melanoma means a higher risk. Some other risk factors include red hair, fair skin, blistering sunburns in the past, or having lots of moles.
Emily Adamek: What are some preventive tips?
Dr. Howard Edington: Avoid the peak hours of sun exposure. If you can’t, wear protective clothing — hats, long sleeve shirts, and long pants. You should also use and reapply broad spectrum sunscreen that protects from UVA and UVB rays. We recommend SPF30 or greater. Zinc oxide and titanium dioxide are the best physical blocking ingredients. They deflect the sun's rays as opposed to chemical sunscreen ingredients that absorb the sun's rays. People are also less likely to have allergic reactions to zinc oxide or titanium dioxide.
You need enough sunscreen to cover your exposed body, and then you want to make sure that you reapply. Application is only effective for about two hours, and if you're sweating or in the pool, you probably need to apply even more often.
Remember to apply sunscreen to spots we often forget about — the ears and back of the ears, the neck and back of the neck, the back of the hands; these are high-risk areas that get a lot of sun. And, even in the winter with the cold and clouds, UV radiation comes through, so wear sunscreen year-round.
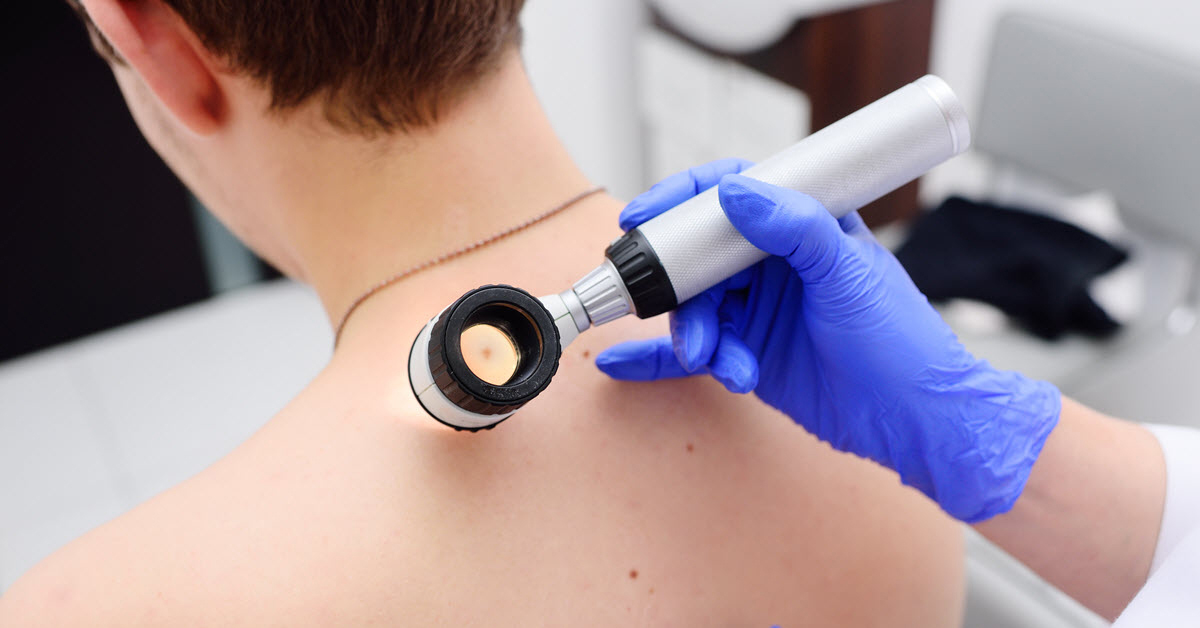
Dr. Edington emphasizes the importance of being screened for melanoma and skin cancer by a dermatologist, particularly if you have risk factors or notice anything abnormal or changing about your moles.
Emily Adamek: What types of screening should people look into for skin cancer and melanoma?
Dr. Howard Edington: Right now, the best screening tool we have is a good set of clinical eyes. A dermatologist can evaluate you, get a family history, and look at risk factors to put you in a risk category. They can then recommend proper surveillance, usually a total body exam once a year, but it could be up to four times a year.
Within the non-melanoma cancer group, there are many patients who need increased surveillance because they have a comorbidity that puts them at a higher risk, or are immunosuppressed, such as transplant patients, HIV patients, patients with rheumatologic problems, and others.
Emily Adamek: What about self-screening?
Dr. Howard Edington: You should look for anything atypical. Maybe you already have many moles, but now you notice one that stands out — that should be checked. We rely on a history of change over time, so if you notice changes, don’t wait, make an appointment. Sometimes, people think because something is small and just on the skin, it can’t do them harm. That’s not true.
Emily Adamek: Is there a typical path from noticing something through diagnosis and treatment?
Dr. Howard Edington: The most common situation is that a person notices something abnormal on their skin and takes a trip to the dermatologist, who would decide either to follow it for a period of time or do a biopsy right away. If a biopsy reveals basal or squamous cell, they will often remove it. If it’s invasive melanoma, they will refer the person to a surgeon.
From there, they usually have surgery to remove the primary lesion and assess any evidence of spread, typically starting in the draining lymph nodes. For patients who have nodal involvement, the prognosis is generally worse. Spread would indicate that there should be additional treatment, including medical oncology and possibly radiation oncology. Radiation is quite effective for non-melanoma, but not so much for melanoma. Patients with melanoma and nodal involvement are seen by medical oncology for systemic therapy, including newer agents such as immunotherapy or targeted therapy.
Emily Adamek: Put simply, would you explain immunotherapy as harnessing the immune system to fight cancer?
Dr. Howard Edington: Yes, but even stated simply, it’s profound — a paradigm shift for treatment. Past drugs were tested and approved to treat a certain type of cancer. With immunotherapy, you may be using a drug to treat a mechanism, common to multiple cancers, as opposed to just one disease. With chemotherapy, you target rapidly dividing cells, which doesn’t only include tumor cells, but also hair follicles, the lining of the GI tract, bone marrow — so it has very non-specific side effects and actions. Newer immunotherapy agents focus on the immune system — which eliminates some of those side effects.
Emily Adamek: You’re one of only a few physicians in western Pennsylvania providing the oncolytic virus treatment using a genetically modified herpes virus. How does that work?
Dr. Howard Edington: Viruses invade cells, and an oncolytic, or cancer-killing, virus is one that has been genetically engineered to identify and infect tumor cells, based on the metabolic differences between tumors and normal cells. The T-VEC treatment uses modified herpes type 1 — the kind that normally produces a cold sore, but now engineered to infect tumor cells only and elaborate a proinflammatory cytokine that magnifies the immune response.
Basically, the virus gets into tumor cells, kills them, and in the process, generates an immune response, which then helps treat tumors even farther away from where you initially injected the treatment. That’s called the abscopal effect.
One of the exciting things we’re looking to do in the future is combine T-VEC with other treatments. It’s been done to some degree, and it looks like it might be synergistic with other cancer immunotherapies.
Emily Adamek: What else is on the horizon of new treatment?
Dr. Howard Edington: We’re hoping to start tumor-infiltrating lymphocytes (TIL) therapy — that’s when we surgically remove a tumor from the patient and grow the cells ex vivo, meaning in a culture preparation. Within that tumor, there are the patient’s own T-cells, which can be energized, then given back to the patient, with the idea being that they will fight the cancer more effectively. The exciting thing is that TIL seems to work in patients who have failed other therapy options. I already used the phrase “paradigm shift” earlier — but this treatment is another one.
Emily Adamek: Do you have plans of doing CAR T-Cell therapy?
Dr. Howard Edington: We hope so, yes. CAR T-Cell therapy with engineered T-cells has been used effectively for hematologic malignancies like leukemia and lymphoma. It hasn’t been as successful with solid malignancies; however, melanoma should be responsive because it has such a rich immunologic history.
Emily Adamek: Is there any other up-and-coming research you’d like to discuss?
Dr. Howard Edington: We’re interested in the interaction between the tumor and what’s called the tumor microenvironment — so, looking at the cross-talk between the tumor and the noncancerous cells around it to find ways to impact the cancer. More generally, I would add that we are really in an exciting, explosive part of what might be called the “research bell curve”!
Emily Adamek: AHN recently announced plans to open a Melanoma and Skin Cancer Center — can you talk more about that?
Dr. Howard Edington: The center has two components — one is research. We’ve covered some of the high points there — therapeutic modalities like the oncolytic virus, CAR T-Cell, and TIL. It’ll also involve some novel ways of imaging, which hopefully make diagnosing melanoma or precursor lesions more objective.
The research component will be contiguous with the clinical component. A key concept there is that we’re providing everything in one place. Patients coming in with a complex problem can see multiple doctors — the surgeon, medical oncologist, support people like navigators and social services professionals, and others. Right now, in most places, you see a dermatologist, then you wait to get in to see a surgeon who might be located somewhere else, then after that, you wait again to get a medical oncology appointment. The biggest burden for a cancer patient isn’t necessarily the treatment, it’s those delays, the stress of waiting and not knowing.
There is a whole set of services we want to build into the center as a response to suggestions from patients. As doctors we have learned about some of these things from our patients, but also specifically through a very nice relationship with the Pittsburgh Melanoma Foundation. The foundation connects with many patient survivors and their families, and they have helped to identify areas for us to potentially develop and improve overall care. We often think of community outreach, but this may be an example of community “in-reach,” and we are excited to make their feedback part of the new center.
Emily Adamek: Looking back over your career, how much has skin cancer awareness and treatment evolved?
Dr. Howard Edington: There is a growing awareness about melanoma in the sense of knowing what to look for, identifying high-risk populations, and recommending appropriate surveillance — the problem being that numbers are still going up.
As I said earlier, advances in treatment have been nothing short of dramatic. However, there is a need for better surveillance techniques. That will be one focus for the center — to develop more objective, machine-based criteria for screening.
If you catch skin cancer early, even melanoma, it’s curable. The Pittsburgh Melanoma Foundation has done a great job of increasing local awareness, and focusing on early detection and machine-based screening is something that seems to work well elsewhere, such as Australia.
When you’re dealing with advanced cancer, if you take a success rate from 0 to 50%, that’s an incredible improvement, but it means 50% of your patients are still dying. The cup is half full, but it’s half empty too, which means there is more work to be done.