When I tell my cab driver I’m headed to Allegheny General Hospital (AGH) to observe a mini aortic valve replacement, he shudders and laughs, “Count me out.” I, on the other hand, am deeply excited. I’ve always been interested in both medicine and surgery, and I jumped at the chance to join a group of high school students as part of the AGH Open Heart Surgery Observation Program.
In the weeks leading up to my participation in the program, I noticed that people run hot or cold on the subject of surgery. They are fascinated — or decidedly not. The 17,000+ students who have participated in the program in the last decade fall into the former category. They sign up because, at this young stage in life, the prospect of a career in the medical field intrigues them.
The observation program was created in 2008 by Dr. George Magovern Jr., system chairman of the Department of Thoracic and Cardiovascular Surgery for Allegheny Health Network (AHN) and co-chair of AHN’s Cardiovascular Institute.
His father, the late Dr. George Magovern Sr., was a pioneer in cardiovascular medicine. He co-created a sutureless heart valve that improved the survival rates of open heart surgery to 90 percent at the time, and helped to establish AGH as a major player in the cardiovascular field.
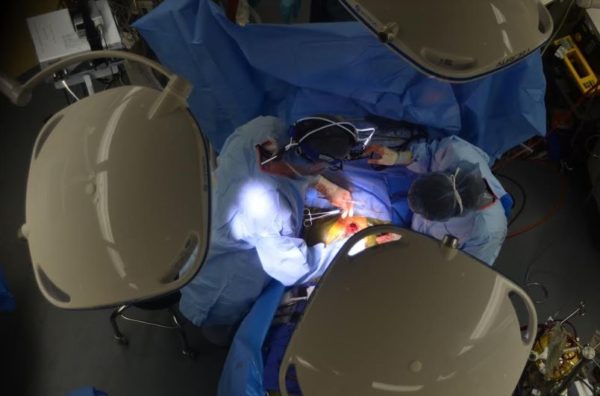
View from the observation room of the patient’s exposed heart.
Before I enter the observation room, Dr. George Magovern Jr. takes a moment to discuss the program with me. He exudes calmness. I’m about to watch something restorative but graphic, and still, his demeanor makes it easy for me to relax.
As a teenager, Dr. Magovern was able to watch his father perform surgery. He felt the same intangible pull toward medicine that these students feel today. Years later, he started the AGH Open Heart Surgery Observation Program because he believed that if kids had the chance to observe surgery, it would inspire them to pursue careers in health care.
“They are all pretty fascinated by the beating heart,” he says, then smiles. “Plus they get to see some blood.”
Observation takes place directly above the operating room. On this day, twelve students from Somerset Area High School and their teacher are already gathered around the raised window when I enter the room. A couple of noses are pressed against the glass.
Dr. Walter McGregor, a cardiac surgeon at AGH, is performing today’s procedure. He wears a camera on his head so that what he sees is projected on a monitor at the front of the room. In addition to the camera, Dr. McGregor wears a microphone so that his voice is broadcast into the room. Unless he speaks directly into the mic, the conversation is muffled. The environment is professional and comfortable.
I look down through the observation window onto a white, sterile room. My eyes immediately find the exposed heart, red and pulsing. It’s hard to shake a sense of tunnel vision. The lack of blood is surprising, but not long after I think this, Pat Wolf, the observation program coordinator, says, “In a moment you’ll see the most blood you’ll see all day.”
A sudden flow of blood appears and is suctioned away. One student laughs nervously. “How much do they lose?”
Standing near the monitor, holding an enlarged anatomical heart, Wolf reassures that it is “not much.” During the visit, she spends much of her time describing functional anatomy and how an operating room, well, operates.
AGH is a teaching hospital for medical students from Temple University, Drexel University, and the Lake Erie College of Osteopathic Medicine (LECOM). The hospital is a proud proponent of early and ongoing education. As an extension of that philosophy, the AGH Open Heart Surgery Observation Program isn’t simply a chance for silent observation. It’s a classroom as well.
“The new valve is most often made from bovine pericardium,” Wolf explains, “which has a lifespan of about 15 years.” She holds up her hands like she’s pinching two ends of an invisible sheet of paper. “As with fabric, they cut leaflets out of the pericardium to make the new valve.”
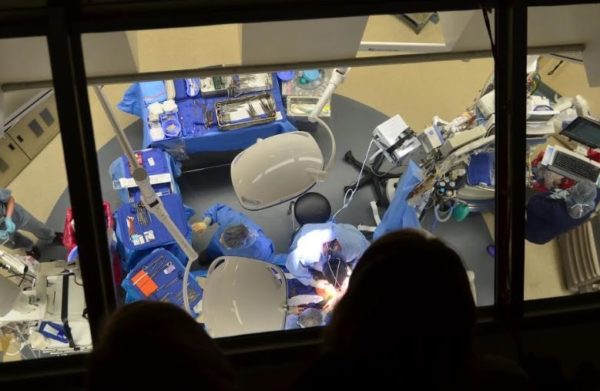
A view of just a few of the 10 team members involved with the surgery.
To perform the valve replacement, the surgical team must slow and stop the heart. They cool the patient’s body down to 64 degrees Fahrenheit and use a cardiopulmonary bypass machine, also known as the heart-lung machine, to temporarily pump and oxygenate the blood.
“It’s very much a team effort,” Wolf says, pointing out the 10 people in the room below involved in this operation. “It’s something for you all to consider — if you choose to go into medicine, you’ll always have a career.”
The students have varied interests. They talk about which roles they see themselves in — anesthesiologist, physician’s assistant, nurse practitioner, or even the perfusionist, the operator of the heart-lung machine.
Surgical procedures and technology have continued evolving at a rapid pace since Dr. Magovern Sr. co-created the sutureless valve in 1963. AGH has continued his pioneering spirit, accomplishing remarkable feats such as implanting valves through the femoral artery and other forms of minimally invasive surgery.
According to Dr. Magovern Jr., 600 operations per year at AGH are what the hospital considers advanced or “cutting edge,” including small-incision, catheter-based and robotic surgeries.
“The field of medicine is wildly dynamic,” Wolf explains. “It’s always moving forward, trying to get better, faster, safer, and less expensive.”
Just to cite one of the many benefits of those constant advances in medicine and technology, a report found that from 2005 to 2015, the mortality rate in heart valve surgery dropped by 47 percent.
Wolf points out the defibrillator in the operating room, but the team doesn’t need the paddles today. I have a bird’s eye view as Dr. McGregor gives the heart a nudge, and then another.
“The heart wants to beat,” Wolf explains. “If you look under a microscope, the cells will beat.”
Sure enough, Dr. McGregor gives one more gentle nudge and just like that, to the sound of someone whistling in the hall, the heart starts to beat again. It’s not dramatic. It’s quiet, easily missed, which makes it all the more impressive.

Dr. Stephen Bailey, a cardiac surgeon at AHN, answers questions from students on another observation day.
As the team begins to close the incision, Wolf tells the story of a patient with an ornate chest tattoo. When the surgical team closed, they took extra time to make sure the abundance of stitches were aesthetically pleasing against the tattoo.
One by one, the surgical team starts to filter out of the room. Still at the operating table, the physician’s assistant looks up and waves.
One of the students voices my thought: “I still can’t picture a real person under there.”
A girl to my left has other things on her mind. “Have you ever heard of someone sewing up with an instrument still inside the body?”
Wolf looks like she’s been asked this question before. “No. This isn’t anything like Grey’s Anatomy.”
Each in their own way, these students feel a sense of awe and fascination, just as George Magovern Jr. felt while watching his father perform surgery many years ago.
After the procedure, Dr. McGregor pays us a visit to answer questions. The students are mostly interested in what path he took to become a surgeon — how did he choose this specialty?
“The specialty you’re good at will draw you in,” he says, engaging us with the same comfortable ease as Dr. Magovern.
“You’re not going to ace everything,” he adds, then laughs. “I mean, you should ace some things. But other things you just have to get through.”
He asks if any of the students were initially spurred to pursue a career in medicine when a family member became sick or injured. A few hands raise.
“Remember your experiences and reflect on them,” he says. “Sometimes illness can lead to the inspiration that makes one want to become a doctor.”
When the questions stop coming, he politely excuses himself, but pauses to nod toward Wolf: “She runs a wonderful program.”
“Certain people are drawn to medicine,” she says. I believe she is referring not only to the students, Dr. McGregor, Dr. Magovern, and the operating team, but to herself as well.
The beauty of a program like this is that it inspires students to open that door of interest. After observing an open heart surgery at AGH, if you want to be in (or above) that operating room, you’ll find a way.

The 12 students from Somerset Area High School who shared my amazing AGH Open Heart Surgery Observation Program experience.