
The AHN Cancer Institute is an emerging national leader in innovative technology, treatment, and clinical research. It is also part of a deeply patient-centered culture that prioritizes improving the experiences of individuals and families across all stages of the care journey.
The interviews in this article are a small sample of the “innovate from every angle” mindset in action. I spoke with Dr. Bindu Rusia about GammaPod®, the world’s first radiation machine designed specifically to treat breast cancer. Dr. John Nakayama shared insights on AHN’s phase 1 clinical trials using tumor-infiltrating lymphocytes (TIL) therapy to treat ovarian cancer. And Dr. Patrick Wagner, a cancer treatment innovator in his own right, showed me that innovation can also be as “brilliantly simple” as a patient-led initiative to develop better, more dignified hospital gowns.
If you’re like me, by the end of the article, you may have a newly expanded definition of “innovation,” along with an appreciation for how these different efforts share the same goal of making a real difference in the lives of people dealing with cancer.
AHN was one of the nation’s first systems to offer GammaPod®, a first-of-its-kind stereotactic radiotherapy system optimized to treat breast cancer. Dr. Bindu Rusia, an AHN radiation oncology specialist, explains that, “GammaPod® uses geometry and anatomy in our favor, in that patients are treated in a prone position — on their stomach.”
Noting that traditional radiation machines deliver treatment with the patient on their back, Dr. Rusia says that having the patient on their stomach means that the breast falls away from the body, allowing for a reduced dose of radiation to the heart, lungs, and body in general.
“The breast is also immobilized with a suction cup,” she adds, “which means we’re able to treat with smaller margins of error, so less breast tissue is exposed to radiation as well.”
With GammaPod®, doctors can deliver treatment for early-stage breast cancer in as few as one to five sessions. In the past, treatment would have taken four to six weeks, often involving time off work and an array of side effects like fatigue and severe skin reactions.
At AHN, a GammaPod® patient can typically expect a total of six visits, the first of which is a consultation. Once they’re determined to be a candidate, they come in for treatment. First, doctors will try different suction cups to determine the best and most comfortable fit. Next, they will get a CT scan while laying on their belly. After some planning from the team, the patient goes into the treatment machine, again on their belly. During the 15- to 20-minute treatment, you can play music or talk to your doctors.
Most patients receive two treatments a week, every other day. They can expect to be in the department for an hour and a half the first day and 45 minutes to an hour on subsequent visits.
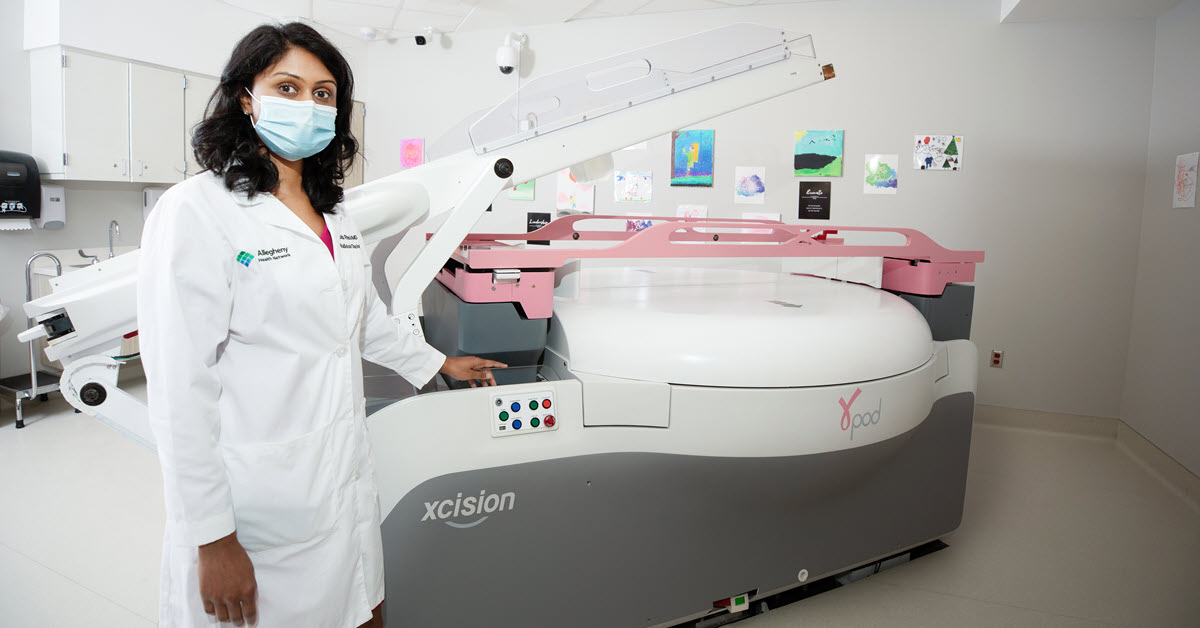
GammaPod® accuracy simplifies the breast cancer treatment cycle, keeps radiation away from a patient’s heart and lungs, and reduces the chance of side effects.
“With something difficult to treat like ovarian cancer, the way to change the game may be to do something different — and we’re harnessing a totally new mechanism,” says Dr. John Nakayama, an AHN gynecologic oncologist who specializes in treating ovarian, cervical, uterine, endometrial, and vulvar cancers.
The new mechanism gaining attention: tumor-infiltrating lymphocyte (TIL) therapy. TIL therapy is part of a Phase 1 trial at AHN that is focused on treating ovarian cancer and also includes some patients with endometrial and cervical cancer.
“There is no real screening test for ovarian cancer, so it can be difficult to detect early,” explains Dr. Nakayama. “All it takes is for one cell to float into your abdomen, and you’re already at stage 3 cancer.”
Between 60% and 70% of people with ovarian cancer are stage 3 or 4 at the time of diagnosis. In those later stages, there is also a high probability of cancer recurring.
Chemotherapies used to treat ovarian cancer can be effective, but with recurrence there is risk of accumulated toxicity, chemo resistance, and other challenges.
“When we talk about chemo, we talk in terms of cycles,” Dr. Nakayama says. “If you’ve had three lines of therapy, we know that with additional lines of therapy, the response rate typically drops to 20% or less. That’s not very good.”
TIL therapy represents a promising alternative. The approach involves extracting lymphocytes — immune cells — from a patient’s tumor, multiplying and “super-charging” them in the lab, and then re-infusing them into the patient.
While the treatment is still in Phase 1 trials, results have been encouraging.
“If you try something novel, it might change the game for someone,” Dr. Nakayama says. “Another positive aspect of this treatment that’s different from traditional chemotherapy is that it’s one and done — it’s just that one infusion of the cells back into your body.”
The idea for a hospital gown redesign emerged from a relationship between the AHN Cancer Institute and a special group of patients who have received treatment at AHN for peritoneal surface malignancy, a form of cancer that spreads to the abdominal cavity and organs. As discussed in past interviews with Dr. David Bartlett, chair of the AHN Cancer Institute, AHN’s use of HIPEC (Hyperthermic Intraperitoneal Chemotherapy) and other innovative treatments can bring hope to patients with difficult cancers like these.
In this case, the patients also became the innovators. After an enthusiastic group of veteran patients, along with some of their caregivers, developed a more formal patient ambassadors group, they gave themselves a challenge: “What can we do that’s innovative and leads to improvements but doesn’t require advanced technology or clinical research?” One initiative that answered that question: Redesigning and improving hospital gowns.
“As is, there’s not a lot of dignity in wearing a typical hospital gown. Often they don’t fit or function very well,” admits Dr. Wagner. “The patient ambassadors decided to change that.”
Among others, Dr. Wagner notes that patient ambassador Bob Granata has used his background in manufacturing car interiors to attack the problem with abandon. He also credits Laurin Scanlon, director of volunteer services at the AHN Cancer Institute, with helping to lead the project forward.
As for the redesign, Dr. Wagner describes it as “brilliantly simple.” It starts with two use cases: a “shirt gown” for people with breast cancer in the outpatient setting for radiation treatment, and a traditional inpatient gown for patients having complex surgery.
It’s easy to see why these scenarios require different accommodations — and why the traditional “one-gown-fits-all” approach causes so much frustration. The inpatient gowns for someone going through surgery, for example, need to function with things like IVs and feeding tubes. They also need to be easy to change while someone is lying flat in a hospital bed.
“This has been an interactive process with different mockups and multiple passes,” Dr. Wagner explains. “The group has spent a lot of time with patients as well as providers, getting their feedback. But, most importantly, this is about the patient’s perspective. If you’re going to spend your day in the hospital or be stuck here after surgery, what things matter to you? A gown fitting and functioning and not causing extra stress becomes very important.”
Although it is not quite ready for mass production yet, Dr. Wagner says the current prototype will soon be tested on the floor. Noting that the patient ambassadors truly are thinking about this from every angle, he adds that the gowns fold up easily like a poncho and will be color-coded for different sizes, so they’re simpler for staff and laundry service as well.