Overview
One of America's leading health insurance organizations and an independent licensee of the Blue Cross Blue Shield Association, Highmark Inc. (the Health Plan) and its affiliated health plans (collectively, the Health Plans) work passionately to deliver high-quality, accessible, understandable, and affordable experiences, outcomes, and solutions to customers.
As the fifth largest overall Blue Cross Blue Shield-affiliated organization, Highmark Inc. and its Blue-branded affiliates proudly cover the insurance needs of approximately 7 million members in Pennsylvania, Delaware, New York and West Virginia. Its diversified businesses serve group customer and individual needs across the U.S. through dental insurance and other related businesses.
In 2022, Highmark Inc. and its affiliate health plans:
- Helped keep patients healthier and generated nearly $700 million in health cost savings through its signature True Performance value-based program.
- Improved prescription drug affordability and accessibility, including by partnering with other leading Blue Cross Blue Shield organizations to lower the cost of generic prescription medications.
- Marked the five-year milestone in a joint venture with Penn State Health. Through the joint venture, Highmark and Penn State Health have created and expanded health care access points throughout central Pennsylvania; partnered with private practice clinicians to improve patients’ health outcomes and lower costs; worked with community-based organizations to combat COVID-19 and improve health equity; invested in leading-edge cancer research; and launched novel health insurance products.
Highmark’s federal programs earn top scores, serve customers and communities

With innovative products, lower costs, and more than 80 years of experience, Highmark remains a trusted name in health care.
For those who don't receive health insurance from an employer, Highmark Inc. and its affiliated health plans (collectively, the Highmark Health Plans) have a range of coverage options that serve everyone — from seniors to entrepreneurs to children, including underserved, vulnerable members of Highmark communities. Highmark's Federal Market programs — including Medicare Advantage (MA), Medicaid, the Affordable Care Act (ACA) marketplace, and Children's Health Insurance Program (CHIP) — are nationally recognized and becoming the insurance option of choice for more individuals and families.
Highmark Health Plans proudly serve more than 345,000 seniors through Medicare Advantage plans. Each year, the Centers for Medicare and Medicaid Services (CMS) evaluates the quality of MA plans using a 1- to 5-star rating scale, taking into account factors such as keeping members healthy and up to date on preventive care measures, managing chronic health conditions, member responsiveness, handling problems and complaints, and customer service. Seniors in Pennsylvania, West Virginia and New York all had the option of choosing Highmark insurance plans that achieved a five-star rating — the highest possible quality score.
Through the work of Highmark Wholecare, Highmark Health Plans' federal-program footprint in Pennsylvania extends beyond Medicare Advantage to include traditional Medicaid and individuals who are dually eligible for Medicare and Medicaid. Total year-over-year membership grew by more than 55,000 in 2022 to nearly 376,000 members. With its 4-star plans, Highmark Wholecare focuses on whole-person wellness with a special dedication to social determinants of health, which are factors like housing, nutrition, transportation, and financial stability that collectively influence up to 80% of a person’s health outcomes. Highmark Health Options, a Delaware Medicaid managed care program, helps more than 164,000 members get the care and services they need to live healthier and more independent lives. In addition, Highmark Western New York provides Medicaid enrollment to 58,000 members in the 8 counties of western New York.
With innovative products and lower costs, the Highmark Health Plans have expanded their Affordable Care Act membership to more than 171,000 members — growing total ACA membership by 65% over the past three years. A signature ACA offering in western Pennsylvania, Together Blue, connects the world-class care of Allegheny Health Network (AHN) with an innovative service and experience model from the health plan.
Highmark Healthy Kids, a CHIP program, serves nearly 16,000 children and continues the organization's legacy of putting kids, families and communities first. When the steel industry collapsed in the 1980s, the company partnered with stakeholders from across Pennsylvania to create a program ensuring that all children, regardless of their family's financial status, have quality health coverage. The program went statewide, and then became a model for the national CHIP program.
With a commitment to put customers first, Highmark, Inc. earned a Brand Excellence Award from the national Blue Cross Blue Shield Association (BCBSA). The annual Brand Excellence Awards honor Blue Cross and Blue Shield plans and are given in recognition of the efforts of Blue Cross Blue Shield plans in building brand strength and providing superior customer service, solid financial performance, and enrollment growth.
Collectively, Highmark Health Plans now proudly serve more than one million customers through federal health insurance programs. With more than 80 years of experience serving members and locally based customer service teams across the region, Highmark remains a trusted name in health care.
True Performance program has recorded nearly $2.5 billion in health cost savings by keeping patients healthier [article]
Other Highlights
- By launching innovative programs and partnerships, Highmark is making prescription drugs more affordable and accessible
- Through community partnerships, provider education and new virtual and in-person treatment options, Highmark restores hope and promotes recovery for substance use disorders
- Highmark saved nearly $1 billion in fraud, waste and abuse over the past five years
- Highmark, Inc. earned a Brand Excellence Award from the national Blue Cross Blue Shield Association, in recognition of building brand strength and providing superior customer service, solid financial performance and enrollment growth

An independent licensee of the Blue Cross Blue Shield Association, Highmark Inc., together with its Blue-branded affiliates, collectively comprise the fifth largest overall Blue Cross Blue Shield-affiliated organization in the country with approximately 7 million members in Pennsylvania, Delaware, West Virginia, and western and northeastern New York.

Star ratings for Highmark and its affiliated health plans: For 2022, Community Blue, Complete Blue, Freedom Blue and Security Blue Medicare Advantage plans in Pennsylvania, and Medicare Advantage PPO plans in western and northeastern New York, achieved the highest possible quality rating from the Centers for Medicare and Medicaid Services: 5 Stars. Medicare Advantage plans in West Virginia and New York Medicare Advantage HMO plans achieved ratings of 4.5 stars.

As of January 2022, Highmark Health Plans had more than 345,000 Medicare Advantage members across Pennsylvania, West Virginia, Delaware, and parts of New York.

With innovative products and lower costs, Highmark has expanded its Affordable Care Act membership to more than 171,000 members — nearly doubling its total ACA membership over the past three years.

The Health Plans are supported by more than 154,000 in-network physicians; in 2022, the Health Plans processed more than 214 million claims on behalf of customers.
Spotlight: Growth Through High-Quality Federal Programs
Through Medicare Advantage (MA), Medicaid, the Affordable Care Act (ACA) marketplace, and Children's Health Insurance Program (CHIP), Highmark Health Plans now serve nearly 1.2 million customers through federal health insurance programs.



 READ MORE
READ MORE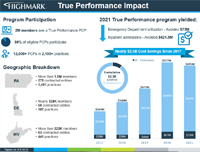









 Share This
Share This DOWNLOAD OUR 2022 CORPORATE PROFILE
DOWNLOAD OUR 2022 CORPORATE PROFILE